What is diabetes?
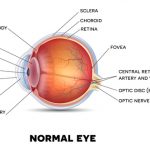 To understand Diabetes, we need to understand the role of insulin in your body. When you eat, your body turns food into sugars, or glucose and at that point, your pancreas then releases insulin. Insulin serves as a “key” to open your cells and allow glucose to enter, which is used for energy. But with diabetes, this system does not work. As a result the glucose levels are high in the blood. This high glucose levels then damages the blood vessels in body.
To understand Diabetes, we need to understand the role of insulin in your body. When you eat, your body turns food into sugars, or glucose and at that point, your pancreas then releases insulin. Insulin serves as a “key” to open your cells and allow glucose to enter, which is used for energy. But with diabetes, this system does not work. As a result the glucose levels are high in the blood. This high glucose levels then damages the blood vessels in body.
Diabetes can affect the eye in several ways.
Diabetes can lead to partial or even total loss of vision.
Diabetic damage to the eye includes:
Retinopathy:
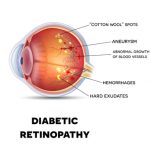 This is caused by damage to the blood vessel in the eye. This is a progressive disease involving the retina. The retina is the delicate light-sensitive part at the back of the eye. It picks up the images, like the film in a camera. Adequate treatment by performing laser photocoagulation can lower the risk of blindness, but often diabetic retinopathy does not manifest itself with loss of vision until it is almost too late to intervene. In other words, if you are diagnosed with diabetes you might be at risk of retinopathy, which you might be unaware of. The only way to reduce the risk of loss of vision due to diabetic retinopathy is to have your eyes checked regularly.
This is caused by damage to the blood vessel in the eye. This is a progressive disease involving the retina. The retina is the delicate light-sensitive part at the back of the eye. It picks up the images, like the film in a camera. Adequate treatment by performing laser photocoagulation can lower the risk of blindness, but often diabetic retinopathy does not manifest itself with loss of vision until it is almost too late to intervene. In other words, if you are diagnosed with diabetes you might be at risk of retinopathy, which you might be unaware of. The only way to reduce the risk of loss of vision due to diabetic retinopathy is to have your eyes checked regularly.
Cataract:
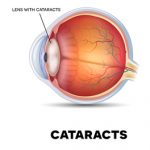 This is more common in diabetic individuals. Diabetes can cause cataracts to develop at a young age and also to develop/progress more rapidly. It can be effectively cured by surgery.
This is more common in diabetic individuals. Diabetes can cause cataracts to develop at a young age and also to develop/progress more rapidly. It can be effectively cured by surgery.
Glaucoma:
 This disease results from increased pressure in the eyes, and can eventually lead to blindness, if not detected in the early stages. This disease may produce no symptoms until a late stage. It occurs more frequently in diabetics.
This disease results from increased pressure in the eyes, and can eventually lead to blindness, if not detected in the early stages. This disease may produce no symptoms until a late stage. It occurs more frequently in diabetics.
How should your eyes be checked?
In order to assess the eyes effectively, the pupils of the eye may need to be dilated. This process involves the use of drops, which may cause sensitivity to light.
When should your eyes be checked?
When the diagnosis of diabetes is made a baseline check must be done. If no damage is found, follow-up examinations should be done once a year.
Treatment
The standard treatment of diabetic retinopathy involves glucose control combined with Argon laser therapy. Laser treatment has been proven to help stabilise any retinopathy, and thus may avert permanent visual loss.
In addition to laser treatment, many patients are now treated with intra-vitreal injections (these are injections given into the core of the eye). It is a relatively painless procedure which can be done under local anaesthetic.
The studies looking at the results of those newer treatments show that many patients not only stabilized, but many will actually improve their vision (this was not the case where patients were treated with laser therapy).
These injections are typically given once a month until the disease process is controlled.
